Keystone
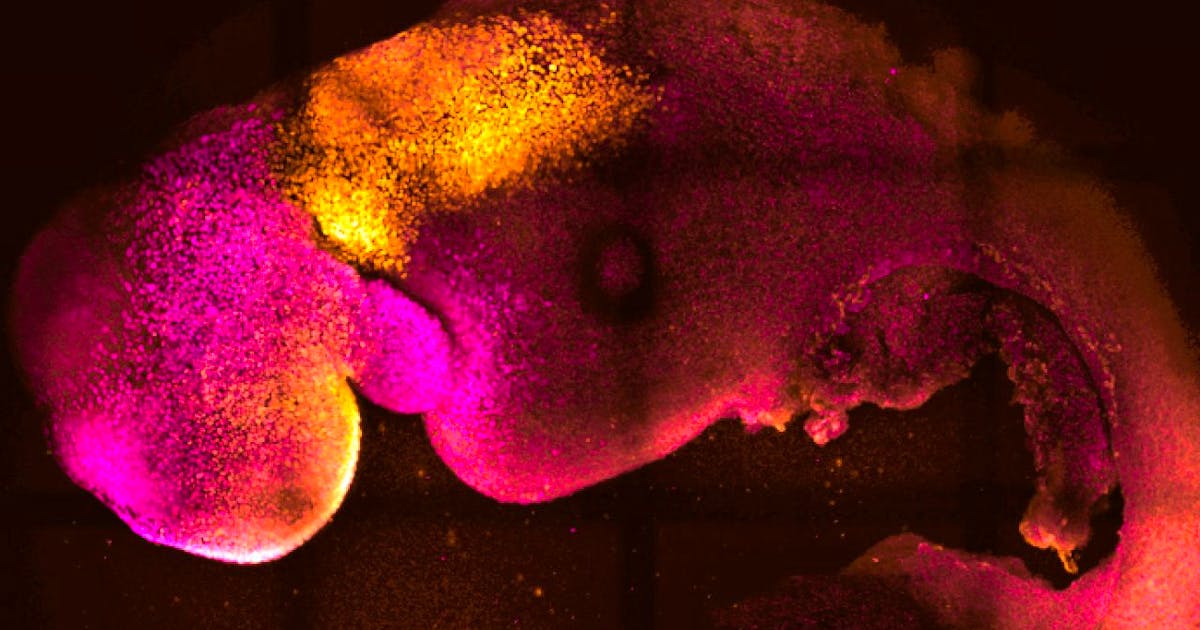
He’s got the first artificial mouse embryo that has reached the record development of 8.5 days, with a beating brain and heart: it’s a living laboratory to understand the failure of some pregnancies and study diseases without testing on animals.
The study was published in Nature by a group of researchers from the University of Cambridge led by Magdalena Zernica Goetz, with Gianluca Amadi (University of Cambridge and Padua) and Charlotte Handford of the California Institute of Technology (Caltech).
In 2017, the same research group obtained the first artificial embryo from embryonic stem cells. Until then it was a mouse embryo, but it was not able to go through all the stages of development.
In this new experiment, a mixture of embryonic stem cells, the brown cells needed to nourish the embryo (trophoblast) and extraembryonic (ETiX) cells, all from mice, was used. The big difference, compared to 2017, is that the researchers were able to get the cells to chat with each other, so that they assemble automatically, without the need for external stimuli.
The fetus develops for eight and a half days, resulting in the formation of a complex and differentiated structure that includes certain areas of the brain, the neural tube that gives rise to the nervous system, a structure similar to the beating heart. Others are similar to the intestines.
A living lab in miniature
In this real, miniature living lab, the researchers also showed that they could reproduce the characteristics observed in so-called lab-knockout mice, that is, deprived of the gene in order to study physiological characteristics or the causes of diseases.
Meanwhile, Caltech reports that the same research group is working on a human embryo model similar to a mouse just obtained and the goal is to be able to understand critical steps in embryonic development that are impossible to observe in real human embryos.
If the technique being tested in mice in the future also works with human stem cells, the researchers say, it would be possible to build organs to transplant to patients on the waiting list in the lab.
“There are a lot of people in the world waiting years for a transplant,” Zernica Goetz says. “What makes our work so exciting is that the resulting knowledge can be used to grow artificial human organs to save lives in the future.” He concludes that transplants “will also help to understand how to make them better and treat them more effectively.”
SDA

“Infuriatingly humble social media buff. Twitter advocate. Writer. Internet nerd.”