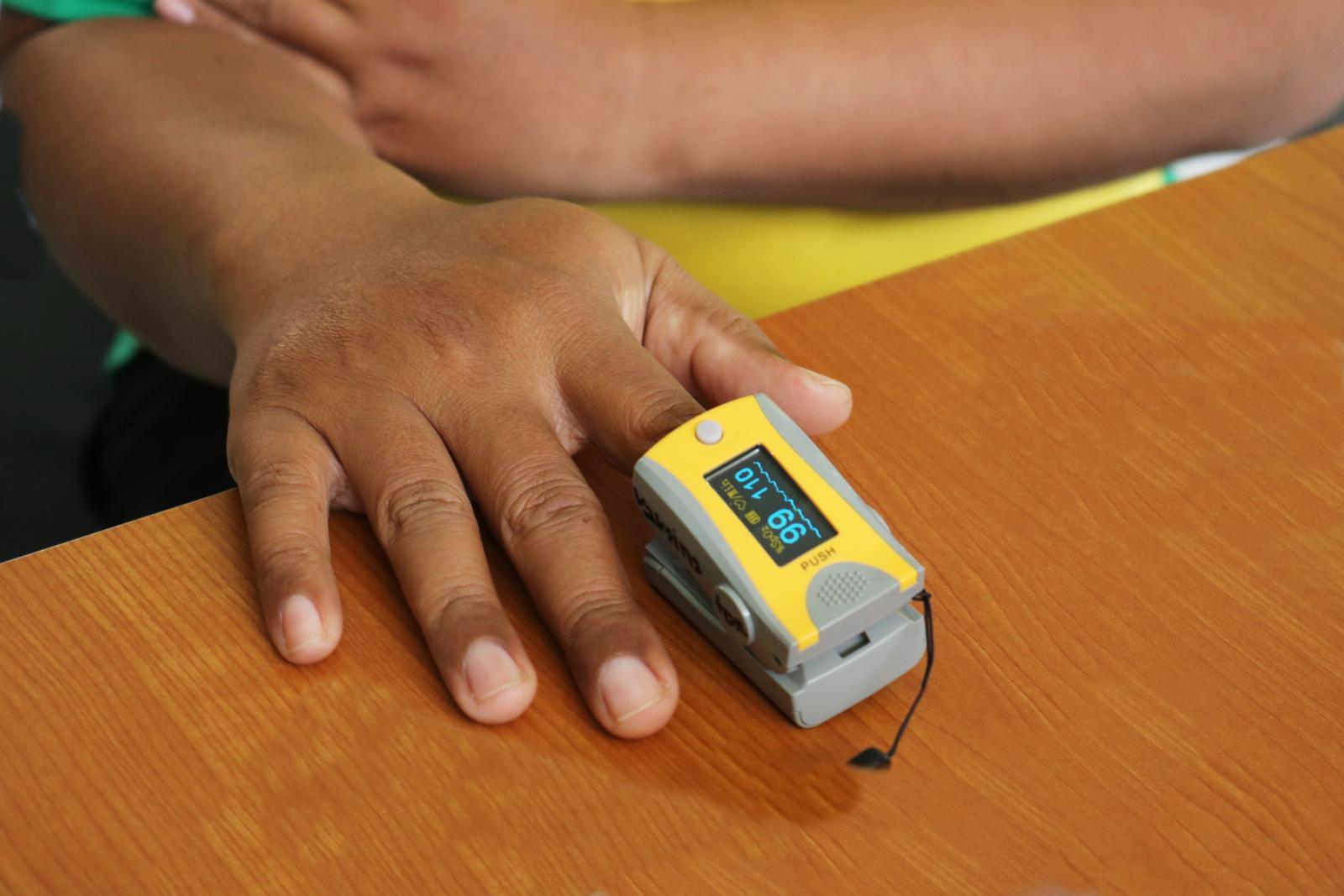
Pulse oximeters or pulse oximeters are instruments that work with the spectrophotometric principle, developed in the 1970s for non-invasive monitoring of patients with respiratory diseases: they calculate peripheral arterial oxygen saturation (SpO2), based on binding absorption and non-hemoglobin Oxygen-correlated to light emitted of two wavelengths (red and infrared) by two diodes touching the patient’s skin and measuring the pulsatile flow of arterial blood (heart rate). An oxygen saturation greater than 95% is considered normal, but it should be considered that the SpO2 value you read on the screen is only an approximation of the true value of arterial oxygen saturation. For example, a value of 90% equals a true saturation between 86 and 94%. Therefore, more predictive weight should be given to the direction of subsequent surveys than to a single identification.
In general, the accuracy of pulse oximeters is good for oxygen saturation at 90-100%, medium for 80-90% and as low as below 80%. In particular, psychological, pathological, iatrogenic, or technical factors can make the estimation of SpO2 erroneous. The latter category also includes racial bias, related to skin color, on which studies have recently multiplied: the largely incomplete bibliography compiled by the author includes three studies published this year (over hereAnd the over here And the over here) who observed, by comparison with the measurement made using arterial blood samples, that in the databases of different hospitals in the United States, such as the pulse oximeter, the more it overestimated the oxygen saturation the darker the skin.
There have already been other reports in the past two years on me gamma And the on me New England Journal of Medicine. By combining all the data, it is evident that in dark-skinned subjects, pulse oximetry gives a systematic overestimate of SpO2 exceeding 1 percentage point which translates to up to 3 times the risk of ambiguously increased and, consequently, untreated hypoxemia. During the Covid-19 epidemic, this “mistake” in the instrument resulted in a 20% lower chance of prescribing a specific treatment for people with dark skin compared to people with light skin: an indication of hospitalization, oxygen therapy, or the granting of experimental drugs (such as remdesivir or dexamethasone) based on the oximetry 94% detected with the device. Thus, the pseudooximetry behavior in non-white ethnic groups could at least partially explain the increased mortality rate from SARS-CoV-2 infection, which has been found in the United States and also in Great Britain, by many of the people tested Well. Studies (eg over hereAnd the over here And the over here).
The unreliability of oxygen saturation estimated by pulse oximetry in dark-skinned subjects, especially at borderline levels, is not a finding associated with Covid-19: it was already verified in 2005 by a study in the magazine Anesthesia It’s again reconfirm in 2007. However, knowing the critical importance is meaningless to acknowledge and take into account, despite the fact that the Food and Drug Administration has recommended that pulse oximeter manufacturers provide representative pre-authorization studies from a demographic point of view, which, i.e. People of all skin pigmentation degrees advertising a marketing program appeared after evaluating the accuracy of the devices for different ethnic groups.
The (racial?) underestimation of the need for oxygen is of interest at present, but it is but one of many health inequalities that will not find solutions in science and in the clinic, however advanced, until they are found in society, i.e. in Politics. For example, it is pointless to resort to proper diet guidelines to prevent metabolic, heart and tumor diseases (yes to vegetables, no to processed foods and sugars) and neglect The reasons why they are being ignored by the most marginalized, the poorest and the least educated. However, the places where the medical literature is lacking is precisely what Socioeconomic and ethnic information On the topics registered in the search.
However, it is not just about wealth or education: In 2002, the innovative report Unequal treatment. Confronting racial and ethnic disparities in health careEdited by a division of the National Academy of Sciences, it revealed that, for the same economic and insurance situation, people of color had significantly less ability than white people to have dialysis, coronary artery bypass and transplants, and more amputations for diabetes. and cesarean delivery, in a measure of variance that surprised the authors of the report. In a detailed article I just published The New York TimesJessica Gross dismissed the same topic of maternal and infant mortality in the United States. The United States is among the 13 places in the world where the death rate from pregnancy or childbirth is higher today than it was 25 years ago; black women They are 3-4 times more likely To enrich this statistic of white children, black children I Often preterm or low birth weight and a mortality rate more than twice that of whites (11.3 vs 4.9; in Italy in 2017 it was 2.75‰) with greater variance now than in 1850, 15 years before abolition. slavery. In the 21st century, a black woman with a college degree is more likely to lose her child than a white girl who just finished high school and has meaning beyond the anecdotal stories that a sports star like Serena Williams had to struggle with before she was diagnosed. Pulmonary embolism after cesarean delivery.
An explanation for this illogical reality was attempted twenty years ago by Arline Geronimus, a professor at the University of Michigan School of Public Health, who first linked maternal and infant mortality to the stress of racial and gender discrimination. Women cannot escape, launching the so-called “atmospheric factors” theory (weathering): The atmosphere of social racism (which includes minimizing symptoms and lack of access to health care) can lead, in a pregnant woman, to high blood pressure and this, if not recognized and treated, to pre-eclampsia, with all the consequences of the cause. How Writes Linda Villarosa, who teaches journalism at City College of New York in Harlem, until it is recognized and combated, the hidden burden of racism will affect the lives and health of Americans.

“Infuriatingly humble social media buff. Twitter advocate. Writer. Internet nerd.”